Medicare improper payments in Fiscal 2013 increased by almost 19 percent, a jump of almost $6.5 billion over last year, according to the most recent Department of Health and Human Services annual report.
Despite the increased attention, scrutiny, and auditing programs aimed at improper payments for Medicare’s fee-for-service programs, the improper payment rate jumped in 2013 to just over $36 billion, the first increase after several years of decline. The HHS annual financial report, dated Dec. 16, revealed that the improper payment rate, which includes payments made as a result of fraud and error, increased from 8.5 percent or $29.6 billion in 2012.
insidePatientFinance.com subscribers can download the entire financial report here: (You must be logged in to download this file. Don't have an account? Register for free and you'll be returned to this page.)
This statistic poses a significant threat to the balance sheets of healthcare providers in the coming three years, because the failure of the Medicare claims processing contractors to detect these errors means 20 percent more job security for Medicare’s cleanup crew, the Recovery Audit Contractors (RACs).
“One of CMS’ key goals is to pay claims properly the first time,” the report states. “This means paying the right amount, to legitimate providers, for covered, reasonable and necessary services provided to eligible beneficiaries. Paying correctly the first time saves resources required to recover improper payments and ensures the proper expenditure of valuable Medicare Trust Fund dollars.”
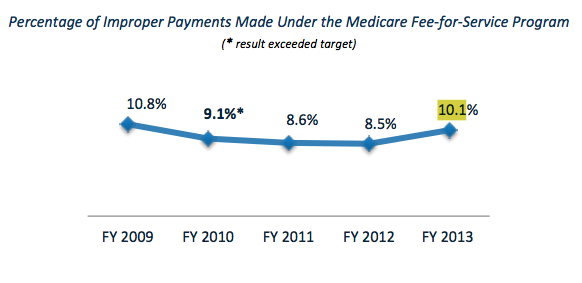
The statistic, which is calculated by the Comprehensive Error Rate Testing (CERT) Program, found that from Fiscal 2009 to Fiscal 2012, the improper payment rate showed a steady decline, but in Fiscal 2013 (which ended Sept. 30), the rate mysteriously shot up by almost 19 percent from 8.5 percent to 10.1 percent. HHS had no explanation for the jump. “Efforts are currently in progress to investigate and resolve the drivers causing this increase,” the report states.
The increase in the improper payment was actually a half percentage point higher, but CMS changed the methodology by not counting those claims that were submitted improperly under Part A and later denied, but then allowed under a change in Medicare policy to be resubmitted under Part B. As explained in the annual report:
“HHS calculated an adjustment factor based on a statistical subset of inpatient claims that were in error because the services should have been provided as outpatient. This adjustment factor reflects the difference between what was paid for the inpatient hospital claims under Medicare Part A and what would have been paid had the hospital claim been submitted as an outpatient claim under Medicare Part B. Application of the adjustment factor decreased the overall improper payment rate by 0.6 percentage points to 10.1 percent or $36.0 billion in projected improper payments.”
There were other changes in the methodology calculating the improper Medicare payment rate, which are outlined in the annual report (pages 162-3). HHS, however, does not attribute the increase to the methodology changes.
The report also states that HHS will work to reduce the percentage of improper payments, but in its projections for the coming years, the percentage decreases but the dollar amount increases by a more than a billion dollars in Fiscal 2014 and 2015, and then jumps $2.75 billion in Fiscal 2016.




![[Image by creator from ]](/media/images/2015-04-cpf-report-training-key-component-of-s.max-80x80_F7Jisej.png)


![[Image by creator from ]](/media/images/Collections_Staffing_Full_Cover_Thumbnail.max-80x80.jpg)
![Report cover reads One Conversation Multiple Channels AI-powered Multichannel Outreach from Skit.ai [Image by creator from ]](/media/images/Skit.ai_Landing_Page__Whitepaper_.max-80x80.png)
![Report cover reads Bad Debt Rising New ebook Finvi [Image by creator from ]](/media/images/Finvi_Bad_Debt_Rising_WP.max-80x80.png)
![Report cover reads Seizing the Opportunity in Uncertain Times: The Third-Party Collections Industry in 2023 by TransUnion, prepared by datos insights [Image by creator from ]](/media/images/TU_Survey_Report_12-23_Cover.max-80x80.png)
![[Image by creator from ]](/media/images/Skit_Banner_.max-80x80.jpg)
![Whitepaper cover reads: Navigating Collections Licensing: How to Reduce Financial, Legal, and Regulatory Exposure w/ Cornerstone company logo [Image by creator from ]](/media/images/Navigating_Collections_Licensing_How_to_Reduce.max-80x80.png)